NC Providers Council Legislative & Policy Initiatives
2025 LEGISLATIVE PRIORITIES
Working in tandem with the Providers Council Board and standing Committees comprised of Provider and Provider Support members, the lobbyists are ensuring that the Providers Council’s legislative priorities are communicated to key Committee Chairs and Members during the 2025 Long Session.
The NC Providers Council has a strong reputation for its analysis of legislation, administrative rules, and Medicaid State Plan, waiver, and clinical coverage policy provisions that impact community services funded through the North Carolina General Assembly and the Department of Health and Human Services (DHHS). We are engaged with General Assembly Members through Maynard and Associates. We also collaborate with numerous Divisions of DHHS – including participation in statewide workgroups and committees, and we maintain an ongoing, constructive dialogue with Standard Plan and Tailored Plan leadership. The association leverages its statewide and systemwide involvement to advocate for providers and the people whom we support.
Legislative Session bill trackers and other documents related to NC Providers Council legislative advocacy are posted on the password-protected Member Communications page.
2025 State Budget Update:
In March 2025, Governor Stein published his Recommended Budget. Health Care priorities and recommended appropriations are listed below. Priorities include direct care workforce program funding, additional Innovations Waiver and TBI Waiver slots, and appropriations for the CMS-approved statewide expansion of the Healthy Opportunities Pilots.
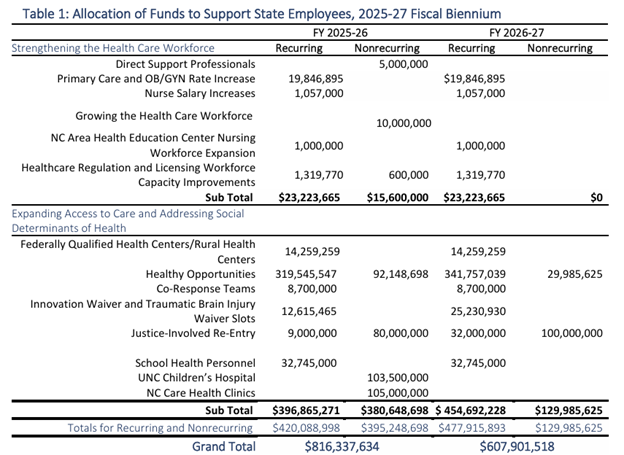
As of April 2025, the Senate referred SB257, an Appropriations Act placeholder bill, to the Appropriations and Base Budget Committee. The Senate budget may or may not reflect the biennium budget recommendations in the Governor’s budget. The North Carolina Providers Council will continue to monitor and update budget bill activity for members in standing committee meetings and on the password-protected Member Communications page.
The Providers Council uses its bi-weekly member policy newsletter and standing monthly and bi-monthly Committee and workgroup meetings to keep members apprised of developments. You can learn more about the benefits of an NC Providers Council membership here.
OLMSTEAD UPDATES
Olmstead v. L.C., 527 U.S. 581 (1999), is a U.S. Supreme Court case that laid the groundwork for people with disabilities to live their lives as fully included members of the community. The case addressed the Americans with Disabilities Act’s (ADA) “integration mandate.” The integration mandate requires that all public entities, including the State of North Carolina, “administer services, programs, and activities” for people with disabilities in the most integrated setting appropriate to the person’s needs. “Most integrated setting” has been defined as one that enables people with disabilities to interact “to the fullest extent possible” with individuals who do not have a disability. Specifically, the case requires states to provide services in the community for eligible persons with a disability when (a) such services are appropriate; (b) the affected persons do not oppose community-based treatment; and (c) community-based services can be “reasonably accommodated.”
In April of 2024, the State of North Carolina published its long-range plan for Olmstead compliance and included the following six priority areas:
- Increase Opportunities for Individuals with Families to Choose Community Inclusion through Access to Medicaid Waiver HCBS;
- Strengthen Opportunities to Divert and Transition Individuals from Unnecessary Institutionalization;
- Address Gaps in Community-Based Services;
- Increase Opportunities for Pre-Employment Transition Services and Competitive Integrated Employment;
- Strengthen Opportunities to Divert and Transition Individuals from the Criminal Justice System and Promote Successful Reentry to Inclusive Communities; and
- Promote Workforce Development, Recruitment, and Retention.
In 2017, the Protection and Advocacy agency Disability Rights North Carolina sued NC DHHS, on behalf of consumer Plaintiffs, regarding Olmstead violations (See: Samantha R., et al. v. North Carolina and the NC Department of Health and Human Services info on the DRNC Website).
One legal remedy in the original 2022 court Order was for NC DHHS to eliminate the Innovations Waiver waiting list over ten years. Another legal remedy was the cessation of all new admissions to ICF-IID facilities and State-operated developmental centers, with the exception of respite and short-term stabilization services.
The most recent Consent Order from April 2024 will be in effect until April 2026.
- The Order requires NC DHHS to advocate at the NCGA for the addition of more Innovations Waiver slots to address the waiting list; however, the Order does not mandate State appropriations.
- The Order does not require the cessation of all new admissions to ICF-IID facilities as the 2022 Order did.
- The Order prescribes the measures to be included in mandatory NC DHHS reporting related to the lawsuit. NC DHHS initiated quarterly reporting in 2025, and you can access that here.
COMING TO THE NC MEDICAID MANAGED CARE MULTI-PAYOR SYSTEM: CHILDREN AND FAMILIES SPECIALTY PLAN
-
-
- In October 2023, Section 9E.22 of the Appropriations Act ( 2023 – 134) became law and authorized and set forth the parameters of the Children and Families Specialty Plan.
- In January 2024, NC DHHS published a revised concept paper regarding the newest Plan, which will be statewide.
- In February 2024, NC DHHS posted a Request for Proposal for contract bids to administer the Plan.
- In May 2024, the NC Providers Council added a Children and Families Specialty Plan (CFSP) standing committee to its array of committees. NCPC provider members with I/DD, MH-SUD, and Child and Family Welfare services participate in the committee since the Plan will serve not only children and youth in foster care, but the whole family.
- In August 2024, NC DHHS announced Blue Cross Blue Shield NC – Healthy Blue Care Together as the contractor for the CFSP. The new plan is projected to go live in December 2025. Learn more about the CFSP here.
-
QUALIFIED PROFESSIONAL EDUCATION WAIVER HISTORY AND STATUS
- In 2013, the General Assembly enacted N.C.G.S. 108A-54.1B. to give DHHS State Plans and Waivers the force and effect of rules. Part (d) of that statute reads, “State Plans, State Plan Amendments, and Waivers approved by the Centers for Medicare and Medicaid Services (CMS) for the North Carolina Medicaid Program and the NC Health Choice program shall have the force and effect of rules adopted pursuant to Article 2A of Chapter 150B of the General Statutes.”
- In 2017, Session Law authorized an expansion of Qualified Professional hiring qualifications to include pre-education work experience in addition to post-education work experience.
- In 2018, the Centers for Medicare and Medicaid Services (CMS) approved this North Carolina Medicaid program State Plan Amendment to “allow all years of both pre-graduation and post-graduation full-time MH/DD/SAS experience to apply to the qualifications required for MH/DD/SAS Qualified Professionals.” The 2018 State Plan Amendment has the force and effect of rule [“NC Administrative Code”].
- In 2019, DMH/DD/SAS promulgated temporary administrative rule amendments to 10A NCAC 27G .0104 and 10A NCAC 28A .0102 to reflect the 2017 Session Law. However, the temporary rule amendments expired within six months. The content linked here is for historical reference only. If you open the two rules today, they will be in their original form and will not reflect the 2017 Session Law. However, because the 2018 State Plan Amendment has the force and effect of rule, the hiring practice of applying both pre- and post-education experience for Qualified Professionals is still authorized.
- In 2020, DMH/DD/SAS obtained Commission on DMH/DD/SAS approval for a “rule waiver” since the temporary rule amendments had expired. The rule waiver expired on 12/31/2021.
- In 2022, DMH/DD/SAS obtained approval for a new rule waiver request. The renewed rule waiver will expire in 12/2023. The rule waiver gives DMH/DD/SAS until December of 2023 to complete the permanent (versus temporary or emergency) rulemaking process so the administrative rules can finally reflect the QP qualification changes authorized in the 2017 Session Law and in the 2018 Medicaid program State Plan Amendment.
- In 2023, DMH/DD/SUS posted the proposed permanent rule amendments for Subchapters 10A NCAC 27G .0104 and 10A NCAC 28A .0102 for a 60-day public notice and comment period that ended on September 1, 2023. The rules were presented for approval at the November 2023 meeting of the Commission on DMH/DD/SUS. The rules were then presented for approval at the December 2023 meeting of the Rules Review Commission in the Office of Administrative Hearings. The rules were approved with an effective date of January 1, 2024.
- 2025: As of April 2025, HB562 filed in the NCGA would, if enacted, amend statutory Qualified Professional staff definitions by adding a category of qualified individuals who “may be a graduate of a community college with an associate degree in a human services field and has two years of full-time or pre- or post-associate degree accumulated supervised mental health, developmental disabilities, and substance abuse services experience with the population served.” The North Carolina Providers Council will continue to monitor and update bill activity for members in standing committee meetings and on the password-protected Member Communications page.
NORTH CAROLINA GENERAL ASSEMBLY QUICK LINKS
- Click here to access NCGA Session Laws enacted during the 2024 Short Session.
- North Carolina General Assembly Home Page with Daily House and Senate Calendars for the 2025 Long Session http://www.ncleg.net/
- You can “find your legislators” by District or County by simply entering your mailing address into the prompt on this NCGA Web page: Representation – North Carolina General Assembly (ncleg.gov)
- NCGA Member Directory
- NCGA Committees https://www.ncleg.gov/Committees
- Fiscal Research DivisionFiscal Research – Fiscal Research Division – North Carolina General Assembly (ncleg.gov)
- Legislative Drafting Division Legislative Drafting Division – Legislative Drafting Division – North Carolina General Assembly (ncleg.gov)
- Legislative Analysis Division Welcome to the Legislative Analysis Division – Legislative Analysis Division – North Carolina General Assembly (ncleg.gov)
2024 NC PROVIDERS COUNCIL STATEWIDE COMMITTEE AND WORKGROUP PARTICIPATION
- Mental Health Coalition
- Developmental Disabilities Consortium
- Substance Use Disorder Federation
- The Coalition
- DMH/DD/SUS Provider Forum
- NCIOM/AHEC/DHHS/NC Coalition on Aging Direct Care Workforce Workgroup
*Some members also serve on LME/MCO Provider Councils and Boards






