Medicaid Transformation
In 2015, the North Carolina General Assembly enacted legislation to authorize a transition to: Medicaid managed care statewide and regional contracts; the creation of the Division of Health Benefits to administer the State Medicaid and NC Health Choice (CHIP) programs (North Carolina ended its CHIP program in 2023 and transitioned enrollees to Medicaid); and the dissolution of the Division of Medical Assistance. The General Assembly has amended the 2015 legislation in each subsequent legislative session to further clarify and appropriate funding for the incremental transition. Clarifications have included Health Plan licensure and solvency requirements in collaboration with the NC Department of Insurance; Health Plan contract provisions, including Medical Loss Ratios and State authority to implement withholds for value-based payment; managed care enrollment mandatory and exempt beneficiary populations; and covered service carve-outs. Please see the relevant Session Laws listed chronologically below:
- Session Law 2015-245 AN ACT TO TRANSFORM AND REORGANIZE NORTH CAROLINA’S MEDICAID AND NC HEALTH CHOICE PROGRAMS
- Session Law 2016-121 AN ACT TO REQUIRE FURTHER REPORTING FROM THE DEPARTMENT OF HEALTH AND HUMAN SERVICES RELATED TO TRANSFORMATION OF THE MEDICAID AND NC HEALTH CHOICE PROGRAMS AND TO MODIFY CERTAIN PROVISIONS OF THE MEDICAID TRANSFORMATION LEGISLATION
- Session Law 2017-186 AN ACT TO CONSOLIDATE THE DIVISION OF ADULT CORRECTION AND THE DIVISION OF JUVENILE JUSTICE INTO A SINGLE DIVISION WITHIN THE DEPARTMENT OF PUBLIC SAFETY, AS RECOMMENDED BY THE JOINT LEGISLATIVE OVERSIGHT COMMITTEE ON JUSTICE AND PUBLIC SAFETY AND TO EXEMPT THE FABRICATION OF EYEGLASSES FROM CAPITATED PREPAID HEALTH PLAN CONTRACTS UNDER MEDICAID TRANSFORMATION
- Session Law 2018-48 AN ACT TO MODIFY THE MEDICAID TRANSFORMATION LEGISLATION
- Session Law 2018-49 AN ACT TO REQUIRE MEDICAID PREPAID HEALTH PLANS TO OBTAIN A LICENSE FROM THE DEPARTMENT OF INSURANCE AND TO MAKE OTHER CHANGES PERTAINING TO MEDICAID TRANSFORMATION AND THE DEPARTMENT OF INSURANCE
- Session Law 2019-81 AN ACT TO MODIFY THE LAWS PERTAINING TO MEDICAID AND NC HEALTH CHOICE AS NEEDED FOR THE IMPLEMENTATION OF MEDICAID TRANSFORMATION
- Session Law 2020-88 AN ACT APPROPRIATING FUNDS FOR THE DOROTHEA DIX CAMPUS RELOCATION PROJECT AND FOR NORTH CAROLINA FAMILIES ACCESSING SERVICES THROUGH TECHNOLOGY (NC FAST); APPROPRIATING CORONAVIRUS RELIEF FUNDS FOR BEHAVIORAL HEALTH AND CRISIS SERVICES, EARLY CHILDHOOD INITIATIVES, AND COVID‑19 TESTING, CONTACT TRACING, AND TRENDS TRACKING AND ANALYSIS; APPROPRIATING FUNDS FOR THE OPERATION OF THE NORTH CAROLINA MEDICAID PROGRAM AND THE IMPLEMENTATION OF MEDICAID TRANSFORMATION; AND MAKING MEDICAID TRANSFORMATION‑RELATED CHANGES.
- Session Law 2021-61 AN ACT TO REVISE THE HOSPITAL ASSESSMENT ACT TO ACCOUNT FOR MEDICAID TRANSFORMATION.
- Session Law 2021-62 AN ACT MODIFYING CERTAIN MEDICAID-RELATED PROVISIONS OF THE 2020 COVID-19 RECOVERY ACT, UPDATING THE MEDICAID PROGRAM BENEFICIARY APPEALS PROCESSES, INCREASING THE AMOUNT OF ALLOWABLE THERAPEUTIC LEAVE UNDER THE MEDICAID PROGRAM, CLARIFYING THE CODIFICATION OF BEHAVIORAL HEALTH SERVICES COVERED BY STANDARD BENEFIT PLANS, AUTHORIZING COVERAGE OPTIONS FOR BEHAVIORAL HEALTH SERVICES FOR POPULATIONS NOT COVERED BY PREPAID HEALTH PLAN CONTRACTS, REVISING THE TRANSFER OF AREA AUTHORITY FUND BALANCES, REMOVING THE RATE FLOOR FOR DURABLE MEDICAL EQUIPMENT, AND MAKING VARIOUS TECHNICAL CORRECTIONS TO THE STATUTES GOVERNING THE NORTH CAROLINA MEDICAID PROGRAM.
- Session Law 2023-7 AN ACT TO PROVIDE NORTH CAROLINA CITIZENS WITH GREATER ACCESS TO HEALTHCARE OPTIONS. [North Carolina implemented Medicaid Expansion in December 2023. See this NC DHHS Dashboard for current enrollment statistics.]
- Session Law 2023-134 AN ACT TO MAKE BASE BUDGET APPROPRIATIONS FOR CURRENT OPERATIONS OF STATE AGENCIES, DEPARTMENTS, AND INSTITUTIONS. [Authorized the Children and Families Specialty Plan and required DHHS to develop performance standard and timely claims payment metrics for Prepaid Health Plans (Medicaid managed care plans).]
- Session Law 2024-34 AN ACT MAKING MODIFICATIONS TO LAWS PERTAINING TO HEALTH AND HUMAN SERVICES. [In early 2024, two LME/MCOs, Eastpointe and Trillium Health Services, consolidated and Trillium was the remaining entity. This law required a new Board structure for Trillium.]
Medicaid Transformation Legislation has also yielded a road map for distinct managed care plans:
- Standard Benefit Plansfor the majority of Medicaid and NC Health Choice beneficiaries (implemented 7/1/2021);
- Tribal Optionmanaged by the Eastern Band of the Cherokee Indians’ Cherokee Indian Hospital Authority for federally recognized Tribal members and Indian Health Service – eligible beneficiaries (implemented 7/1/2021);
- Tailored Plansfor high-risk, high need populations including but not limited to I/DD, TBI, SMI, and SED (implemented 7/1/2024); and
- Children and Families Specialty Plan for foster care and former foster care populations and their family members (projected for 12/1/2025).
See this NC DHHS Dashboard for aggregated and stratified NC Medicaid managed care plan and Fee-for-Service system enrollment. Plans must use care management to deliver integrated, whole-person care that coordinates physical and behavioral health services with one, statewide Preferred Drug List for pharmacy benefits.
CMS approved North Carolina’s 1115 Demonstration Waiver in October of 2018 with effective dates of January 1, 2019 through October 31, 2024. CMS approved a five-year renewal application for the Demonstration Waiver in December 2024. See the detailed description of continuing and new services here. Changes to the Demonstration Waiver since 2019 have included the 2023 addition of a 1915(i) State Plan Option for the services of Individual and Transitional Support for community living; Individual Placement and Support for employment; Respite; Community Transition; and Community Living and Supports and Supported Employment for qualified Medicaid beneficiaries. In the 2024 waiver renewal, CMS also approved a statewide expansion of the regional Healthy Opportunities Pilots that addresses Social Determinants of Health / Health-Related Social Needs.
Medicaid Transformation has also necessitated State Plan Amendments and the procurement of numerous Health Plan and tangential vendor contracts for Transformation planning and implementation. You can access related RFPs and RFAs here.
North Carolina Providers Council members are committed Behavioral Health, IDD, Substance Use Disorder, and Child and Family Welfare providers and stakeholders in this ongoing system transformation. Association members serve Medicaid beneficiaries and State-funded individuals under a service delivery system of managed behavioral health care through closed network contracts with four regional Tailored Plans administered by Local Management Entity / Managed Care Organizations (LME/MCOs) that serve all 100 NC counties.
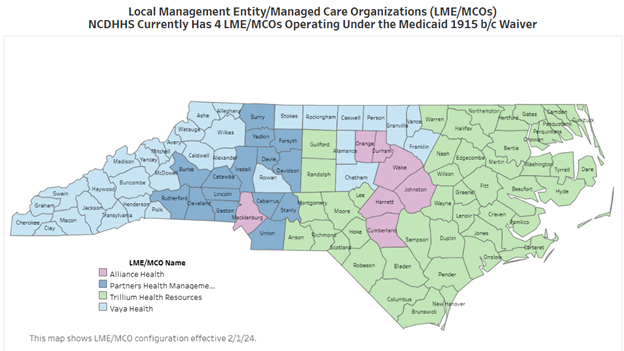
In addition to contracting with Tailored Plans, providers may contract to render services with Standard Plan networks for beneficiaries with mild-to-moderate BH & SUD service needs. Association provider members may also contract with NC DHHS to serve individuals who are currently carved out of the Medicaid managed care 1115 Waiver and in the Fee-for-Service “Medicaid Direct” system. Carved out individuals included Dual Eligibles (Medicare-Medicaid) and individuals who are enrolled in the Community Alternatives Program for Disabled Adults (CAP/DA) and the Community Alternatives Program for Children (CAP/C). The CAP waivers are administered by NC DHHS under Social Security Act Section 1915(c) authority. In addition to Tailored Plans, the LME/MCOs exclusively administer the Innovations Waiver, which is a 1915(b)/(c) waiver for home- and community-based services for individuals with an IDD who qualify for institutional care but want to receive services in an HCBS setting.
The North Carolina Providers Council closely monitors all legislation and other documentation related to Medicaid Transformation and continually communicates policy updates to members. The Providers Council maintains a collaborative relationship with NC Medicaid managed care plans and State Officials, and sponsors opportunities for members to have a dialogue with representatives during standing Committee meetings, at membership leadership forums, and at the annual conference. Furthermore, some Providers Council Board members are also active members of LME/MCO Boards or Provider Advisory Councils.
Listed below are “Quick Links” for accessing NC DHHS and Division of Health Benefits documentation related to Medicaid Transformation.
North Carolina Medicaid Quick Links
State Resources
- Medicaid Transformation NC DHHS Information Portal
- NC Medicaid Clinical Coverage Polices
- NC Medicaid PDL
- NC Medicaid Fee-for-Service Fee Schedules [Note: FFS rates serve as the floor for Medicaid managed care plan rates; in-network providers are paid at least 100% of the FFS rate and out-of-network providers are paid 90% of the FFS rate.]
Federal Resources
- Centers for Medicare and Medicaid Services 1115 waiver information
- Centers for Medicare and Medicaid Services Code of Federal Regulations[See 42 C.F.R. Part 438 for Medicaid Managed Care specifically]
- Title XIX of the Social Security Act[Medicaid Program]

